Carotid Body Tumor: Symptoms, Diagnosis, and Treatment
A carotid body tumor is the most common paraganglioma involving the head and neck. Paragangliomas are tumors that arise from a particular type of cells surrounding blood vessels or nerves.
What are Carotid Bodies?
To understand carotid body tumors, you must have an idea of the carotid body. The carotid body works as a sensory organ made up of different receptors. It lies where the carotid artery divides into external and internal branches.
The receptors of carotid bodies receive information about the blood’s oxygen and carbon dioxide levels. After receiving the appropriate signal, they help regulate the respiratory rate and blood pressure.
Carotid body tumors typically occur in the 4th to 5th decade of life, with a slightly higher incidence in females.



What is Carotid Body Tumor?
A carotid body tumor is the most common paraganglioma involving the head and neck. As the name indicates, it arises near the bifurcation of the carotid artery. A carotid body tumor is critical as it affects the brain’s blood supply.
The patient complains of significant swelling on the side of the neck. Everyone has two carotid arteries that run through the neck’s sides and divide into branches to supply brain and face tissues. In about 10% of individuals, carotid body tumors may involve both carotid arteries.
What are the Causes of Carotid Body Tumor?
In most cases, the cause of carotid body tumors is unknown. Carotid body tumors are rare and often seen in middle-aged or older people. Carotid body tumors are also more common in people who live at high elevations. The driving factor behind carotid body tumors in such people is low oxygen levels in the environment. However, some familial cases of the disease are reported with a history of similar conditions in some family members.
A carotid body tumor is part of a genetic syndrome in familial cases. Some of the important ones are,
- Multiple Endocrine Neoplasia (MEN) syndromes
- Neurofibromatosus Type 1 (NF 1)
- von Hippel-Lindau Disease (vHL)
What are the Associated Symptoms?
The major problem associated with carotid body tumors is their insidious nature. It progresses subtly but may lead to very harmful effects. Most carotid body tumor patients usually don’t complain of any symptoms. However, they may notice a swelling at the side of their neck, which is not painful in most cases.
Symptoms only occur when the tumor enlarges to a size that starts compressing surrounding structures. Some of the common symptoms of sizeable carotid body tumor involve,
- Pain in the throat
- Difficulty in swallowing
- Hoarseness
- Visual disturbances
- High blood pressure or palpitations
How to Diagnose a Patient with Carotid Body Tumor?
Your doctor will confirm your diagnosis based on three parameters. First is the medical history, which involves information about your complaint related to your condition. Next, your doctor will ask several questions related to the problem.
Second, he will physically examine your head and neck and look for positive signs of a carotid body tumor.
In the end, your doctor will need some investigations to confirm the diagnosis. Most investigations involve imaging techniques such as ultrasound, CT scan, and magnetic resonance imaging (MRI). Your doctor will also advise you on a particular type of MRI that visualises your blood vessels, called magnetic resonance angiography (MRA). He will also order some blood tests and might ask for some genetic studies.
However, the confirmed diagnosis is only possible after the excision of the tumor and its examination under the microscope. Therefore, microscopic features are the primary criterion for establishing a definitive diagnosis of carotid body tumor.
What are Different Grades of Carotid Body Tumor?
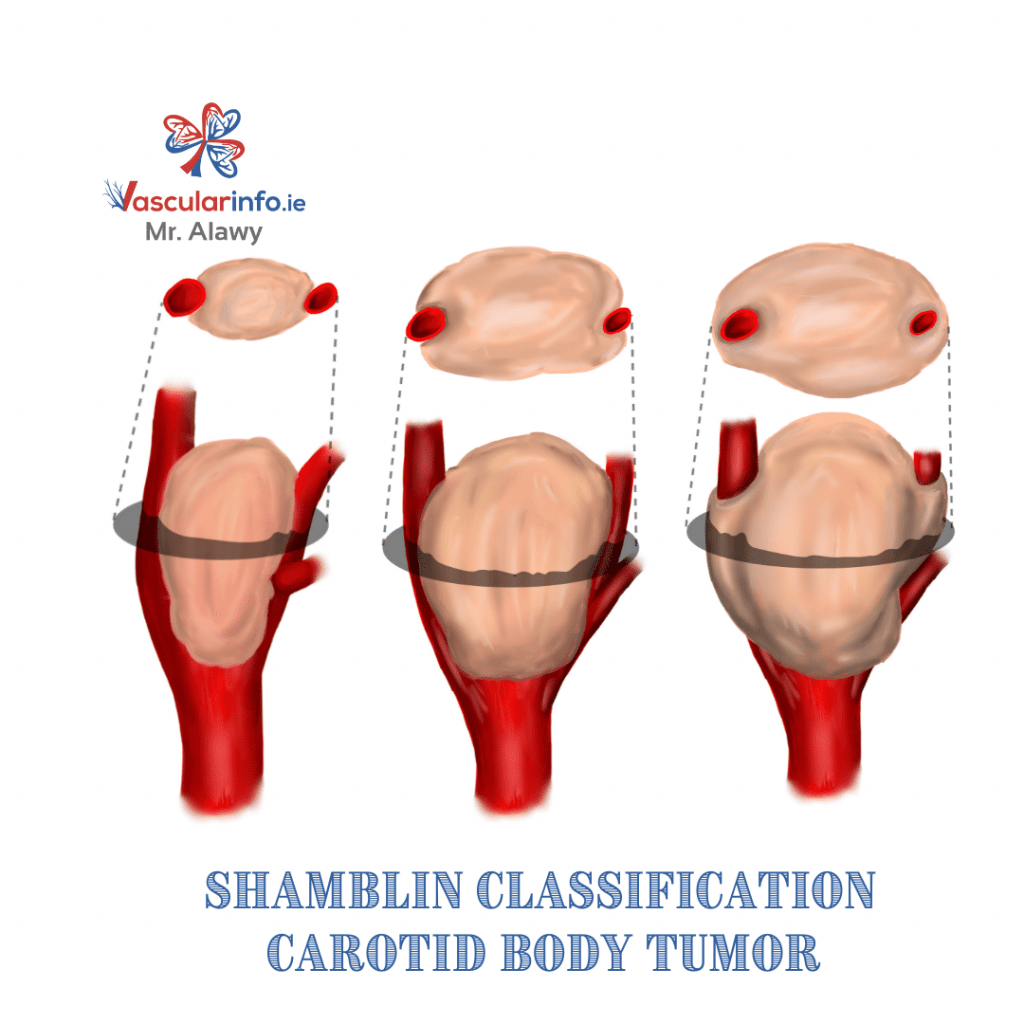
The grading of the carotid body tumor depends upon the circumferential involvement of the carotid artery. The increasing severity and size of the tumor also correspond to the grade. According to a well-accepted Shamblin classification, carotid body tumors can be of three grades.
- Grade I: Grade I carotid body tumors are small and only minimally involve the carotid vessels.
- Grade II: Grade II tumors are larger and encircle a bulk of the carotid artery but do not completely encase it.
- Grade III: Grade III carotid body tumor entirely encompasses the carotid vessels. They are also of the highest severity.
What Does the Management Involve?
Patients usually present complications when the tumor sufficiently increases in size and compresses the surrounding structures. In that case, surgical excision of the mass becomes necessary to prevent damage to neighbouring tissues. In rare cases, radiation therapy is used.
What are the Surgical Options of Treatment?
The tumor does not simply involve the blood vessels. Treatment is usually tailored to each patient after a multidisciplinary meeting dissection with different specialities, including your vascular surgeon, (ENT) surgeons, radiologists, oncology, and endocrinologists. Some patients may benefit from Transcatheter embolisation 2 to 3 days before resecting the tumor to block the artery supplying the tumor. In this procedure, the intervention radiologist will insert a catheter in the groin artery and guide it to the supplying artery of the tumor. Then he will block the artery to decrease the risk of bleeding during surgery.
The surgeon will remove the tumor with special instruments. Then, depending on the tumor size, he may remove part of the carotid artery and replace the artery section with a bypass graft to maintain the blood flow to the brain.
Are There Any Risk of Surgical Treatment?
The risk of surgery varies from one patient to another depending on the tumor size, relation to surrounding structures, and the patient’s fitness. Therefore, your surgeon will discuss your risk in detail before the surgery.
Surgical resection of the carotid body tumor is usually a safe procedure. However, in about 2% of cases, stroke can occur. Stroke risk is higher in patients with large tumors who need vascular repair after the resection.
As already mentioned previously in the article, a tumor also involves nerves. Therefore, removing the tumor can damage the nerves and lead to paralysis or weakening of the supplied structure. However, permanent nerve damage is rare and occurs only in 5% of the patients.
There is a chance of re-development of the tumor in 5% to 10% of the patients. It can reoccur in the same artery or the artery on the other side.